The numbers are so high. I don't understand why there is this "drastic shift" when really if you read toward the end of this article, it discusses ways to prevent the spread of the bacteria. It's basic, common sense actions like washing your hands frequently, use bleach when cleaning, ect. Shouldn't the hospital staff do this no matter what for harm reduction purposes?
Just like the fungal meningitis outbreak that could have been completely prevented if they followed protocol. It all comes down to people being CARELESS. CARELESSNESS KILLS. Those 23 people should be alive today, but because of ad decisions made by people in the position to call the shots, these people didn't make it and many got very sick.
I'm really getting sick of reading stories like this. I'm getting sick of our medical system and how the billion dollar drug companies use unlawful ways to profit more $ (kickbacks people...its gotten corrupt because everyones motivation is wrong).
Just everything ...I'm sick of the crazy prices of medictions these days. Im extremely pissed off that doctors don't even discuss or look at family history/genetics before they jump on suggesting possibly deadly medications. Biologic drugs ARE NOT for everyone.....(like me.... cancer runs on both sides of my family..& guess what kind of cancer? The exact type of cancer that the manufacturer reports that people have gotten from treatment with Biologics. When a doctor just casually mentions that I should be on one of these drugs, it makes me want to punch them in the face.
I ask them exactly what I want to know when I'm there. This is our lives people. Don't ever be intimidated by the man wearing the white coat with a medical degree. Most of them shouldn't even have the degree. Anyone can be a doctor these days. There are brilliant doctors out there.... but finding them is either difficult because of persons' location and require some $ because the doctor is extremely far. Most people won't want to have that burden and will just settle with the stupid man that thinks he's smart. LOL I'm done venting now. Carry on with the article. You'll probably be just as disgusted as me.
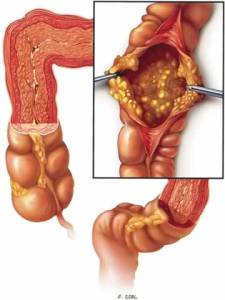 C-DIFF.... IS UGLY!
C-DIFF.... IS UGLY!
Researchers See Dramatic Shifts in C. Diff Infections - Yahoo! News:
 '
'
Just like the fungal meningitis outbreak that could have been completely prevented if they followed protocol. It all comes down to people being CARELESS. CARELESSNESS KILLS. Those 23 people should be alive today, but because of ad decisions made by people in the position to call the shots, these people didn't make it and many got very sick.
I'm really getting sick of reading stories like this. I'm getting sick of our medical system and how the billion dollar drug companies use unlawful ways to profit more $ (kickbacks people...its gotten corrupt because everyones motivation is wrong).
Just everything ...I'm sick of the crazy prices of medictions these days. Im extremely pissed off that doctors don't even discuss or look at family history/genetics before they jump on suggesting possibly deadly medications. Biologic drugs ARE NOT for everyone.....(like me.... cancer runs on both sides of my family..& guess what kind of cancer? The exact type of cancer that the manufacturer reports that people have gotten from treatment with Biologics. When a doctor just casually mentions that I should be on one of these drugs, it makes me want to punch them in the face.
I ask them exactly what I want to know when I'm there. This is our lives people. Don't ever be intimidated by the man wearing the white coat with a medical degree. Most of them shouldn't even have the degree. Anyone can be a doctor these days. There are brilliant doctors out there.... but finding them is either difficult because of persons' location and require some $ because the doctor is extremely far. Most people won't want to have that burden and will just settle with the stupid man that thinks he's smart. LOL I'm done venting now. Carry on with the article. You'll probably be just as disgusted as me.
Researchers See Dramatic Shifts in C. Diff Infections - Yahoo! News
Minnesota scientists studying the records of discharged hospital patients found some dramatic shifts in the infection Clostridium difficile. This germ is commonly referred to as C. diff.
The Mayo Clinic says its researchers examined five years of data from the National Hospital Discharge Study. They found that incidents of C. diff infections among two groups -- children and the elderly -- are becoming more frequent and are increasing in severity.
Of an estimated 13.7 million hospitalized children, 46,176 had C. diff infections. When compared to those without the illness, they had longer hospital stays, more surgeries for removal of part or all of the colon, more stays at long- or short-term healthcare facilities, and a greater risk of dying.
The scientists also followed 1.3 million adults who were in the hospital with C. diff. Those older than 65 experienced longer stays, were sent to nursing homes more frequently, and had a higher risk of dying than others. The researchers concluded that being older than 65 is an independent risk factor for negative outcomes linked to the infection.
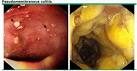
C. diff is a bacterium that causes diarrhea and can result in serious intestinal conditions, according to MedlinePlus. Its most common symptoms are fever, watery diarrhea, nausea, loss of appetite, and/or abdominal pain or tenderness. The disease typically spreads in hospitals, nursing homes, or in other institutions.
The Centers for Disease Control and Prevention reports that C. diff causes 14,000 U.S. deaths a year. The annual tab for treating it is at least $1 billion. The risk of recurrence after one infection is 20 percent. After multiple episodes, it rises to 60 percent.
Individuals who have taken antibiotics are particularly at risk. These drugs destroy beneficial flora in the intestine. Ironically, the main treatment for C. diff is antibiotics, typically oral metronidazole or vancomycin.
The Mayo Clinic states that despite the dramatic shift in these infections, several preventive measures are effective. They include washing hands frequently with soap and water, separating hospitalized patients with C. diff from others without the infection, cleaning surfaces with chlorine bleach, and equipping hospital staff and visitors with disposable gloves and gowns when around infected patients. When antibiotics are necessary, probiotics can help rebalance the intestines.
I have had at least three episodes of C. diff. Years ago, a gastroenterologist advised that patients with Crohn's disease -- particularly those like me on immunosuppressants -- are at elevated risk of contracting it.
I recently developed an infection in my foot that wouldn't go away. After 10 days of an antibiotic, I had several symptoms of C. diff. Since I take metronidazole periodically for Crohn's, I wondered if the bacteria might finally be resistant to it. I bypassed the drug. Each day for two weeks, I took a probiotic and ate yogurt. Fortunately, I avoided yet another C. diff infection.
Vonda J. Sines has published thousands of print and online health and medical articles. She specializes in diseases and other conditions that affect the quality of life.
 C-DIFF.... IS UGLY!
C-DIFF.... IS UGLY!Researchers See Dramatic Shifts in C. Diff Infections - Yahoo! News:

